This is a 14-minute read.
Any healthcare professional who works with lymphedema is familiar with the basic stages of the disease and how it typically presents in most patients. However, massive localized lymphedema (MLL) is a rare form of the condition that’s far less often diagnosed.
MLL is a type of soft tissue lesion that arises primarily after a patient experiences an impact of physical trauma. It’s found almost exclusively in obese patients, usually in the person’s upper inner thigh.
In this article, we’ll review how to recognize MLL, why it’s more common than you might think, and what it’s like to be diagnosed with it from the patient’s point of view. We’ll also explore treatment options that improve a patient’s quality of life.
A Shocking and Difficult Diagnosis
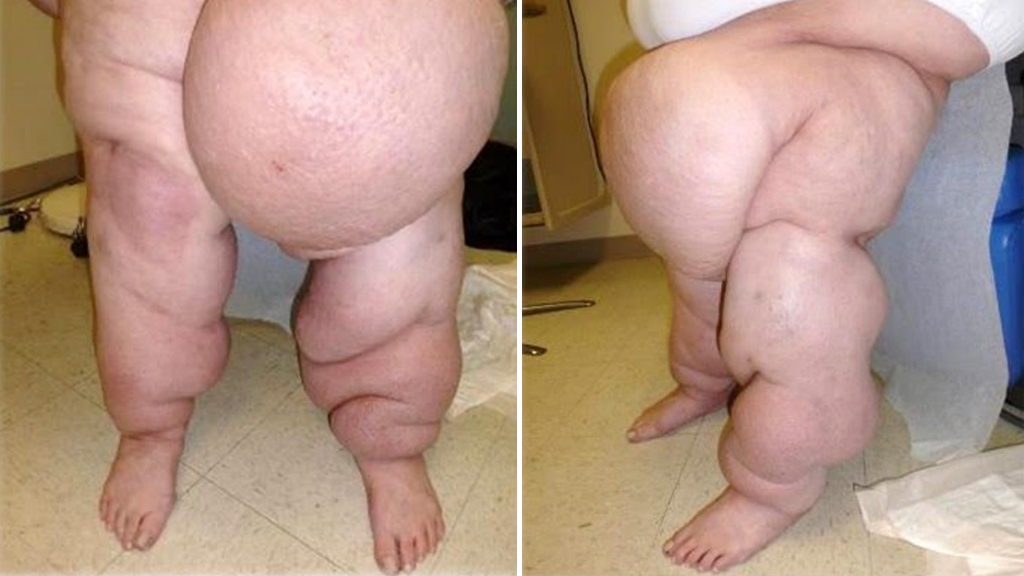
For patients and healthcare professionals alike, MLL can be a rather shocking sight. It has a rough, asymmetrical appearance that is usually indurated (firmer than the surrounding tissue).
Patients are understandably worried about the enlargement but it may have been present for years before you see them, and “massive” is often an accurate term. They have been called “pseudosarcomas” because the mass can be mistaken for this fatal type of cancer that can arise from nearly any type of tissue. While a biopsy is usually the way to confirm that a collection of lymphatic tissue is not cancer, performing a biopsy in an area of MLL can cause a non healing wound that drains copiously. In most cases, the diagnosis can be made clinically and the best approach is to initiate compression to see if the mass reduces in size as expected. It is also possible to obtain an MRI if clinicians involved in the patient’s care feel uncomfortable with a clinical diagnosis (assuming the patient can fit into an MRI).
Unfortunately, many MLL patients often look for help for years before anyone familiar with lymphedema sees them. The MLL collections affect function but generally do not create a healthcare crisis unless a wound develops from trauma or pressure. One unfortunate patient who was only 29 but weighed almost 600 pounds, burned herself on a waterbed heater. She developed a wound and subsequent cellulitis which became a vicious cycle of abscesses, infections and draining ulcers that dripped constantly. We were able to surgically remove almost 100 pounds of pannus, or tissue growth, from her body. Open wounds in an area of MLL can be nearly impossible to heal.
Important Points About MLL Diagnosis
Rare diseases, by definition, occur in fewer than 200,000 people in the U.S. and are uncommon to see in a doctor’s daily practice. MLL is a rare disease that occurs almost exclusively in the morbidly obese, a group that is commonly thought to be about 5% of the U.S. population.
However, in my practice, nearly 10% of our patients are morbidly obese, and a significant percentage of them have MLL which suggests that it can’t be as rare as once believed.
Also, consider how the U.S. population is changing in terms of obesity, which is steadily on the rise. In the 1990s, a 350-pound patient was very rare. However, today it’s become more common to encounter patients who are 600-plus pounds.
Patients are often ashamed of these enlargements and try to hide them but they are usually too large to be hidden by clothing. It is important to examine obese lymphedema patients carefully because MLL can form in the supra-pubic area and scrotum as well as the upper, inner thigh. They are usually unilateral, meaning they only occur on one side of the body, if they are on an arm or leg.
Remember, MLL wounds don’t have a “typical” appearance because the superficial skin is affected by the amount of trauma or rubbing they sustain. If they are surgically removed, histologically they exhibit lobules of fat interrupted by connective tissue. Swelling and inflammation are present but those are characteristic of lymphedema.
Published data on the MLL collections describe them as having a mean diameter of 50 centimeters, and surgically removed MLL masses typically weigh 2,000 to 12,000 grams. However, I’ve found they can be smaller or larger than this. The size can be impressive. I have seen MLL collections that are the size of a beach ball attached to the medial thigh which virtually prevent ambulation.
Why Do MLL Masses Form?
In terms of the pathogenesis of MLL, we assume that it’s caused by lymphatic pathways becoming blocked, but that explanation is unsatisfying. Why they form exactly where they form and why they often recur after they are excised is a mystery. Since they are heavy, gravity affects the blood flow out of the mass and it is common to see changes of venous insufficiency (venous stasis) in the skin caused by leakage of red cells out of the vessels and the deposition of iron oxide pigment, which we call “hemosiderin.”
The enlargement of MLL masses is usually slow but progressive and patients will seek help once they can no longer tolerate the impact to function. For example, one of my patients had an MLL wound develop near his scrotum in the suprapubic area. Eventually, he had to move it out of the way to urinate, which was of course a frustrating and embarrassing problem.
Treating Massive Localized Lymphedema
It is possible to remove the masses surgically and that would seem the logical solution. Strangely, the collections often recur at the same spot. Additionally, if the weight issue is not managed prior to surgery, it is not likely that the patient will have long term improvement. Bariatric surgery should be done first if possible, and after significant weight loss, the MLL will be easier to manage. Removal of MLL masses is usually considered cosmetic and thus not usually covered by insurance. When the MLL involves a very large abdominal pannus, it is possible to perform what is called a panniculectomy in which only the skin, subcutaneous tissue and fat are removed. This is different from a “tummy tuck” because the muscles are not touched. It’s a challenging surgery because the blood vessels tend to retract into the fat and the patients are at risk of significant blood loss. Also, there are dramatic fluid shifts in the body when a huge mass is removed that can weigh as much as 100 lbs. A lot of skill is required to create a cosmetically acceptable closure and the wounds are at high risk of dehiscence due to the generally poor perfusion of fat. Few surgeons are willing to tackle such a potentially problematic procedure.
This case demonstrates the pitfalls of surgical removal of MLL. The patient was only 22 and had a very large collection of MLL removed from one leg. She went home and later gained 125 pounds. Although she then underwent gastric bypass surgery, when she returned to see me she had developed MLL collections on both medial thighs. Her case shows the importance of having bariatric surgery before MLL-related surgery, which is a standard recommendation in cases like hers.
It is important to emphasize that other treatment methods such as compression and manual lymphatic drainage (MLD) can be effective — and more effective than you might think! However, it is very hard to do a compression wrap around what may be a “ball.” Additionally, some collections hang down in such a way that the lymphatic return is blocked. It takes a highly experienced and creative therapist to work with these patients, but it is possible to improve the situation. Naturally it is easier if intervention is done early. This patient demonstrates the importance of early diagnosis and intervention. When you examine two legs side by side and one has been treated with compression from the beginning and one has not, it’s easy to see that the compression-treated leg is smaller.
In the 22-year-old patient described above, the fact that she hadn’t been wearing her compression garments added to the severity of her MLL. Compression wouldn’t have cured her MLL, of course, but it may have prevented it from becoming so much worse. Patients should be instructed how to care for the skin properly to reduce the likelihood of ulceration and subsequent infection.
It’s impossible to effectively address MLL until we also address the underlying issue of obesity. Obesity is a complex disease which has genetic components. There are patients with genetic disorders for which obesity is a feature. For example, those with a genetic condition called Prader-Willi syndrome have a strong predisposition to obesity and Type 2 diabetes. The satiety center in their brain is broken and they have an uncontrollable urge to eat. Someone with this condition has comorbidities that must be considered before settling on a particular form of MLL treatment.
These are the kinds of cases that show the complexity of treating MLL and the need for a thoughtful, comprehensive approach. People with MLL find the condition to be extremely frustrating and are eager for doctors to make as much progress as possible on finding effective treatments.
Finally, it’s important to keep in mind that people who have MLL often struggle with weight, health, and body image issues. This is why I support the concept that The Beauty Still Remains after a diagnosis like MLL. You’re welcome to visit my blog and learn more about the strength and beauty of bodies with massive localized lymphedema.
About Caroline Fife
Caroline Fife, MD, FAAFP, CWS received her bachelor’s and master’s degrees from Texas A&M University College of Medicine. She worked in family medicine at the University of Texas, Southwestern, and served as a member of the faculty of the University of Texas Health Science Center in Houston for 23 years and is now a professor of Geriatrics at Baylor College of Medicine in Houston, TX.
She initiated the renowned Memorial Hermann Center for Wound Healing and the Memorial Hermann Center for Lymphedema Therapy and is currently the Medical Director of the CHI St. Luke’s Wound Clinic in The Woodlands, TX. She’s also the CMO of Intellicure, a Texas-based software company, as well as the director of clinical research for the U.S. Wound Registry. She worked with Eva Sevick to develop real time lymphatic imaging.
For More Information
This article is presented by Lympha Press, world leaders in pneumatic compression devices that support positive health outcomes for people living with lymphedema. Lympha Press offers solutions for patients of all sizes, including the innovative LymphaPodⓇ that adapts to any body size from 350 to 700+ lbs.